The day that changed my life!
A day in early May 2017………………….
It was early morning and the first intravenous drugs of the day were already making their way into my veins, when there was a knock on the door. It was unusual for another knock so soon; it was too early. I knew the routine as I had been in this solitary hospital room for ten weeks.


The nurse walked in. One of my favourites, a quiet yet very kind and caring older nurse of Filipino origin. “You’re going to get a call in a moment” she exclaimed, not wanting to appear too excited. “The call?” I responded, with a hint of surprise in my voice. “Yes” she said, still not wanting to reveal any more. She did not have to, for at that moment the small black phone on the sideboard did indeed ring. It was an unfamiliar buzzing noise. ‘Well, it worked’ I thought, as I lunged across the bed towards it, trying not to strangle myself on the oxygen lead that was supplying the gas through the cannula on my nose.
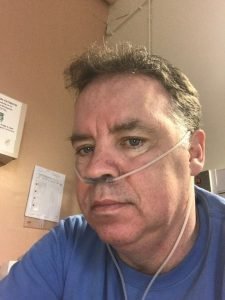

Yet I was all fingers and thumbs and, in my sleepy excited state, I could not find the answer button. ‘Missed call’. I had to laugh. I had been carrying this little phone around with me wherever I went for the past 14 months and the one moment that it rings, indeed the first time that it had ever rung, and I missed the call!
Fortunately, my ‘normal’ phone rang in seconds and the news was good. “Mr Watson, we’ve been offered a set, they look as though they could be good. We don’t know for sure yet, but we’ll get you over here straight away”.
My ten week stay in Room 11 was potentially coming to an end. A moment that I had been waiting for since my admission back in early March 2017, yet a ‘call’ that I had been waiting for since March 2016. There was no time to wait and reflect. A few essentials packed, a few quick goodbyes to the staff on the early morning shift and I was on a trolley and being whisked off into a waiting ambulance.
The lights were flashing as we worked our way through the early morning traffic in London’s West End, red lights ignored, it was something of a blur. A surreal conversation followed with the ambulance girl, recently recruited from Sydney with 200 others to work in the London Ambulance Service. Small talk was strange, it was difficult to put into words and to explain to a complete stranger the magnitude of what was potentially about to happen.
Having spent over 48 and a half years of living with this condition, life had really become something of a struggle. For years it had been amazing, doing everything, well almost everything and living life to the full. Not that it had been without sacrifice, for the daily routine of physiotherapy and taking copious quantities of medication every day, as well as more latterly, numerous nebulised treatments, is both time consuming and restrictive, but these were a small price to pay for an extended life with infrequent hospital stays.
Yet in recent years, and largely as predicted, my ability to function and move around was becoming seriously compromised. I had become completely reliant upon oxygen and, as hard as I tried, I could not really do much about it. I had to accept the position I found myself in, and make the most of it. I kept smiling and being as positive as possible but when I found that I could not even have a shower without becoming completely exhausted, even with oxygen, and furthermore, often having to seek assistance to put my socks and shoes on, life was becoming somewhat frustrating at times.
The Blue Badge had been a godsend in terms of getting to places but even then, getting out of the car and walking around was becoming awfully difficult.
I know that people live with far worse. I was the last to complain but there comes a time. Hopefully this was going to be the right time for me.
As the ambulance made its way out of suburbia into the green fields, my mind turned to my family.
Firstly, and arguably most poignantly, my younger brother Nic. He had the same condition as me, yet he never received the ‘call’ and tragically died on 22 September 2001 at the age of 29. He had suffered more than me throughout our lives yet even so, it was a massive shock that he lost his life at such a young age. From that day onwards, I knew that what I was potentially about to go through now would, more than likely, be my only saviour at some point in my life. That moment had now arrived, over 15 years later.
As a result, and in a strange way, whilst being slightly apprehensive naturally, I did not fear this. Maybe I should have but this was my big opportunity and somewhat curiously perhaps, I wanted to embrace it, telling myself to stay calm and be relaxed. ‘Carpe diem’ is the phrase that is engraved on Nic’s headstone, and those two words rang loud in my head, seize the moment and make the most of this opportunity. This might be my only chance, if indeed I get the chance at all.
Secondly, my wife, parents and sister. My wife Loretta had taken my call earlier whilst on the commuter train to London. She sounded equally calm, alighted at the next stop and retraced her steps home, to drive to meet me at the hospital to which I was being transported. My parents, Allen and Laraine, who I had also telephoned at about 7.30am, had agreed that they would stay at home and wait for news. I wondered what were they going to do all day. Then my special little sister, Victoria, who just had to continue her daily work routine as a solicitor in a busy London practice, likewise waiting for updates as and when.
Thirdly, my extended family, close friends and work colleagues, some of whom we had made aware of me having received the ‘call’ that very morning. So many special people who mean so much to me and who I was so looking forward to seeing again and enjoying life with once more.
In a strange way, I felt quite calm. Whilst I was not really in control of my destiny, at least I knew what was going on at all times, for the moment anyway. For everyone else, it is the ‘not knowing’ that causes the stress and anxiety. It felt like I had the easy bit and I was confident. This was the place to go. These were the experts in their chosen field. Success rates were high. I could only think of the positive and what this could all mean to me and my life. Failure was simply not an option in my mind
As for everyone else, who knows? It cannot have been easy. It is natural to think or fear the worst, it is only human nature after all, despite trying to be as positive and upbeat as possible. I could only hope that my relatively relaxed and calm demeanour would have rubbed off on the others but deep down it can be another matter entirely.
Indeed, as I reflect, maybe the situation was worse for my close family only a few months earlier on a Friday afternoon in early March, when I had taken a massive downturn and was rushed into hospital in an extreme emergency. Now that was quite scary, even for me. Blue lights and an ambulance driver working the roads like a Grand Prix driver, my condition very serious and my memory of that trip sketchy to say the least. I survived that scare but it really was quite worrying all round. That was a pivotal moment in many ways and action really needed to be taken as a result of that occurrence.
I was ‘woken’ from my thoughts by the driver calling out to say that we had arrived. There was no particular rush this time, now that we had reached our destination.
I was ‘wheeled’ into a room, bloods and observations taken once more and it became something of a waiting game. An unusual waiting game. The chances of success could not realistically be predicted. I knew that. Some people get lucky first time, others do not. It is simply the luck of the draw. I could not build my hopes up too much but I was secretly hoping. It would have been disappointing to have to go through all this again but then again risks cannot be taken for something of this magnitude.
The day seemed to take an age. No more food or drink after 12 noon, bar occasional sips of water. The clock ticked slowly. It was difficult to focus on anything. Visits from the coordinator and the nurses were regular but uninformative for they had nothing new to say. Messages back to the family were short and sweet, ‘no news’
That was until shortly after 5pm when Tom, the coordinator, entered the room with a broad beam across his face. “Good news” he exclaimed. “We’re good to go, I’ll go and organise the chariot”. It was an unusual choice of words but I liked it, this was going to be no ordinary bed or trolley but something really quite special, or so it felt to me.
Almost two and a half hours later, having been body shaved, to much amusement and frustration all round, and then showered, I was placed into my chariot and we began the journey downstairs.
The holding area was designed to be a calming experience. Birdsong twittered away in the background, a wall of slowly moving floral designs interchanged with soothing colours. You had to hand it to the team, they had thought of everything. Tom had handed over to his colleague Nicky by now and she did her best to keep me calm. I said ‘goodbye’ to Loretta and in I went.
This was it. Nicky spoke to me and explained what was happening as I was transferred onto a new chariot, strapped in, lines inserted and then anaesthetised. She sensed my nervousness and held my hand to reassure me. My eyes began to close. The clock on the wall in front of me showed that the time was approaching 8pm. My eyes closed……..
Fast forward 32 hours. My eyes slowly re-opened. “Well I’m still here” was my first thought. “That is very good news”. Maybe something of an understatement.
I took in the scene. A large room. Just me and a nurse, who was closely observing my every move. Machines surrounding me. Digital displays with bright numbers monitoring and recording my every breath. Lines everywhere and inserted into seemingly every part of my body. A ventilator helping me breathe. Clearly this was still all very serious. I had never been in an Intensive Care Unit before yet strangely perhaps, there was a certain calmness about everything.
“What time is it?” I asked the nurse. “3.45” she said. “On Thursday?” I responded. “No, Friday” she said.
Gosh, I have missed a day I thought, as I rapidly tried to calculate how long I had been asleep. I was reassured that this was standard practice for an operation of this nature and nothing to worry about. All had gone well.
I was advised that I had briefly woken about 12 hours previously in something of a daze and had wanted to know all about what had happened. Not only that, but apparently I kept repeating the same question in quite an aggressive manner on several times thereafter, even though the nurses had explained to me on numerous occasions exactly what had gone on. ‘Crazy boy’ I thought, ‘how embarrassing’. They had sympathy and let me off, mitigating circumstances I guess.
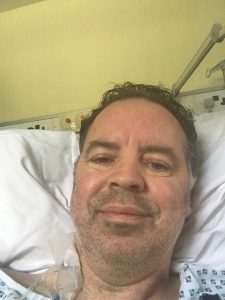

Intensive Care lasted four days; the High Dependency Ward lasted almost two weeks, which included a quick bronchoscopy to clear out some unwanted fluid and also removal of the drains; the ‘Preparation for Going Home Ward’ lasted another week or so where I began walking around and working out on the exercise bike and then, four weeks later I returned home………. with my new lungs.
Epilogue
December 2017
Seven months after my transplant and with my recovery going so incredibly well, I decided to ask my coordinator for more details about my donor. Regulations stipulate that hospitals are only permitted to tell a recipient of a transplant their donor’s age and sex. I had asked the question three weeks post my transplant but my coordinators, quite rightly in my opinion now, suggested that it would be best to wait until I was well on the road to recovery before I found out more details.
In my mind, and perhaps naively, I had just assumed that my donor was an older man, who had lived a full life and had just died of natural causes. That view possibly helped me at the time, so I could just focus on my own recuperation.
So you can imagine my complete shock and unbelievable sadness when I found out that somewhere a girl in her early 20’s had died, in the prime of her life. Furthermore, my thoughts immediately turned to her family, and maybe a partner, and friends, who would no doubt have been completely devastated. Despite my joy at my new situation, I could not help but feel incredibly sad at what had happened to such a young girl and to all of her family and friends. I can only thank her for deciding to become an organ donor and her family for agreeing for her organs to be donated upon her death, for evidence suggests that so many families decide not to when put in this position in the immediate moments after the death of a loved one.
What has happened to me is nothing short of a miracle yet it has only been possible because of this ‘unknown’ girl. I have never met her, will never meet her, I don’t know her name but I think of her every day and will do so forever.
May 2018
Twelve months after my transplant and I returned to Harefield Hospital to attend a charity fundraising launch event, hosted by the Royal Brompton and Harefield Hospitals Charities Trust. It was a really interesting evening and showcased the outstanding work of the Trust as well as that of the Transplant Team at Harefield Hospital, the location of the first heart transplant performed in the UK and arguably the leading heart and lung transplant hospital in the country.
It was a day of reflection and celebration in so many ways, for it really has been a quite an amazing year.
From where I was, with my lung function being at figures of 17% and 35% of the predicted readings of a ‘normal’ person of my age, weight, height, size etc and hence being completely oxygen dependent to, at the latest count, 125% and 111% for the same breathing tests, it really is quite incredible and beyond my wildest dreams.

I have been very lucky in so many ways and it has allowed me to quite literally have a new life. Life is simply amazing with my new lungs. I can now walk for miles, I can run again, I can live a completely full life again and I do feel like a youngster. Who knows what’s around the corner, for I am aware that there is always a chance of ‘rejection’ at some time. However I am, and will continue to give my new lungs my best shot.
Reflection
For those growing up with Cystic Fibrosis (CF), which is what I was diagnosed with at birth, as well as other lung conditions and diseases, there is huge hope for the future. Not only have there been huge medical advances in treating CF during the course of my lifetime, which has enabled me to have a very good quality of life until my early to mid-forties, there is always the possibility of a lung transplant when health worsens. It is quite literally a life saver and an incredible feat of medical technology, performed by hugely talented and skilled surgeons and their teams of medical professionals.
The whole transplant process, from making that initial decision to go on ‘the list’, to waiting, to receiving the call, to the day itself and to the recovery thereafter is not without stress, anxiety and worry. However, the medical teams who have looked after me at both the Royal Brompton Hospital and subsequently, Harefield Hospital, are so incredibly professional, thoughtful and caring, and they really made the whole process as easy as they possibly could. Whilst I cannot deny that I experienced a certain amount of pain in my initial recovery period, this was managed as well as possible and within a week or so, I felt so much better and the initial pain was really a small price to pay.
I recognise that I have been very lucky in terms of having a successful transplant on my first opportunity, the quality of lungs that I have received and how quickly I have recovered.
As I approach my 50thbirthday in September this year, I can now look forward to hopefully leading a full life for many years to come. It really is the greatest gift.
Thanks
Firstly, in addition to my donor, her family and the support of all my family and friends, I must thank everyone who has dealt with me from within the NHS. They do often get criticised, but from my own personal experiences of living with a condition such as Cystic Fibrosis all my life, and then having the transplant, they have been so kind, caring and attentive, I could not really have asked for more.
Secondly, a huge thanks specifically to the Cystic Fibrosis team at the Royal Brompton Hospital in Chelsea, where I have been cared for both as an outpatient and inpatient for the past 33 years.


They have provided excellent care and treatment throughout my time there and are always accessible, offering a very specialist and personal level of care. They are righty regarded as one of the best specialist CF centres in the UK and are at the leading edge of research and new treatments. Professor Margaret Hodson led the way in the earlier years, followed more recently, in terms of my own personal care, by Dr Khin Gyi, Dr Nicholas Simmonds and Dr Andy Jones, with the support of their fellow Doctors and physicians. Dietitian Sarah Collins has provided invaluable advice on diet and diabetes control over the years and, to complete the drum roll, the physiotherapy team led by Helen Parrott, with special mention for Zelda Beverley and Charlotte Gray in more recent times.



Thirdly, for my transplant, the surgeons and all the team at Harefield Hospital have been amazing. Consultants Dr Martin Carby and Dr Anna Reed lead the Transplant and Respiratory Medicine team and it is they and their colleagues who I have dealt with most, both pre and post transplant. They all have exceptional knowledge and experience. On the day of the transplant itself, it was the Transplant Coordinators Tom and Nicky who made the day special and eased my nerves.
Yet it is not just the doctors, surgeons and coordinators who make the whole process run as smoothly as possible, but the incredibly knowledgeable, skilled, caring and loyal nursing and support team who are the ‘glue’ who keep everything together. The same can be said for the nurses at the Royal Brompton Hospital too.
Whilst I have only got to know, and be in the care of, the Harefield team for the past couple of years, it really is a special place. It resembles a ‘cottage’ hospital in many ways because of its size and specific nature of its function as a specialist transplant centre and has something of a family feel. The team get to know you and are rooting for your recovery and wellbeing. It is what they do and they are exceptionally good at it. Long may it continue.


What a fantastic story from a brave & courageous human being
Brilliant well done
Keep smiling as you always do
Also as you said behind every great man is a even better lady Loretta xxx
Peter xxx
Andrew you are amazing. Such an inspirational read. We all thank that young lady for being a donor x